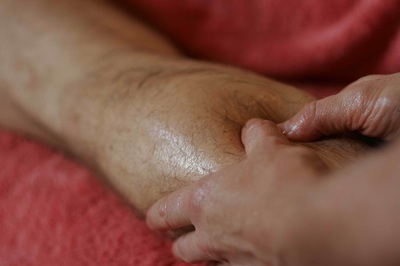
 I'm not one to subscribe to a lot of toys or gadgets to provide treatment and help my clients reach their goals but I do get excited when I find one that works and works really well. Thanks to fellow physical therapist, Erson Religioso, I now have in my possession an excellent new tool, The Edge, that makes my job easier and more effective which is great news for my clients. It may not look like much (or it may frighten some people) but it is an excellent all around tool for Instrument Assisted Soft Tissue Mobilization (IASTM). As much as I enjoy using my hands, there are times when a tool or instrument can really be a huge advantage and difference maker. There are also some tissues in the body that fingers and hands simply cannot have as much of an impact on like metal or other hard objects can. Since The Edge is a 'Jack of all trades' with its variety of edges, it can be implemented in many ways depending on the specific needs of each client and situation. That means having the ability to match the appropriate edge for treatment and truly target the particular issue at hand. The beauty of it is just like many soft tissue techniques, it can be utilized for both prevention and/or treatment for injuries. Admittedly, it saves my hands for other treatments and techniques as well. With its versatility, The Edge can be used for a wide range of issues like tendonitis/tendinosis, muscle strains, trigger points, etc. It can be used for acute or chronic scar tissue formation especially following surgical procedures so that movement and mobility can be restored. Persistent or chronic muscle tightness (think calf and upper trapezius) tends to respond quite well to IASTM. Any type of restriction in connective tissue like the plantar fascia, iliotibibial band, and joint retinaculums are also prime candidates for tools like The Edge. As you can see, there are many applications for IASTM as it can be the perfect adjunct to other techniques and treatments to help you move better, feel better and live better. Sometimes it can the missing piece to help you get over the final hurdle that has been a challenge to get over otherwise. If you have any soft tissue issues or just want to stay ahead of the game with preventative treatment, don't miss out on this opportunity. It really can be a game changer! Knowledge = Power; Share The Power:
0 Comments
 Perhaps. At least it is for mice as of a 2011 study. (1) It is not a perfect connection to make to humans but the conclusions from this particular study are not farfetched either. To this day, it remains a favorite study of mine because the implications of it involve one of my favorite things: Dark Chocolate. At this point, it is no secret that dark chocolate can provide a number of health benefits. Some of these include being an excellent source of antioxidants and several minerals like iron, magnesium and copper as well as being linked to lowering the risk of heart disease, improving HDL and LDL values, and improving blood flow. (2) Flavonoids (or flavonols), chemical compounds found in plants, the cocoa plant in this case, have been implicated in a number of studies as being critical to many aspects of human physiology including the aforementioned examples. A particular flavonol called (-)-epicatechin (known as 'minus' epicatechin), which is present in dark chocolate, has garnered attention over the last several years and was the target of interest in the 2011 study involving mice. Twenty-five mice were randomly split into four groups: 1) water only, 2) water and daily exercise, 3) (-)-epicatechin only, and 4) (-)-epicatechin and daily exercise. All of the mice performed a treadmill test on day 0, underwent their assigned intervention over the course of 15 days and were tested again on the treadmill. The group that received (-)-epicatechin and daily exercise showed significant improvements in all outcomes but boasted an almost 50% increase in distance compared to their initial treadmill test. In comparison, neither of the water groups showed improvements on the treadmill test and actually performed worse overall compared to their initial test. A surprising outcome was the group that received (-)-epicatechin only also performed extremely well. Their treadmill test was nearly as good as the group who exercised. Upon further examination of the two (-)-epicatechin groups, it was discovered that there was a significant increase in capillarity (blood vessels) in skeletal muscle as well as an increase in number and size of mitochondria (the energy factories of cells) in skeletal and cardiac muscle. As with the treadmill test, the group that received (-)-epicatechin and exercised showed the most change but again, even (-)-epicatechin only showed significant changes as well compared to the water groups. In short, this means the mice were able to deliver more blood (read: oxygen) to their muscles and produce more usable energy than their counterparts who only received water. It is no wonder then that they were able to run longer and farther, and fatigue at a slower rate.  So what conclusions can we draw from this? Considering the similarities of skeletal and cardiac muscle among mammals, it is entirely plausible that (-)-epicatechin found in dark chocolate could have the same effect on humans as it does on mice. Clearly the greatest benefit was coupled with exercise but even that wasn't necessary to gain results. Since both groups showed significant improvements, there doesn't appear to be a major advantage of timing your dark chocolate intake. As long as you eat it daily, you will have consistent levels of (-)-epicatechin in your system. It is important to note that all dark chocolate is not created equal. If you plan on adding this to your diet, dark chocolate with higher percentages of cocoa (cacao) will have more (-)-epicatechin so you may want to look for 70-75% or higher depending on your tastes. The only downside that I foresee is that this does not mean you can eat dark chocolate until your heart is content, which is a true shame. The levels administered to the mice would equate to rather small portions, on the order of a half to a full square per day for humans, in order to have the same desired effect. Unfortunately, more is not better in this case. This type of self control and will power may be difficult for some but the potential benefits could really prove to be performance enhancing. What is not known is whether these types of physiological changes plateau after a certain amount of time or if it would even have an effect on those who are already at a higher level of fitness. Either way I'll take my chances since dark chocolate is absolutely delicious to begin with and at the very least I can take advantage of the other health benefits it has to offer anyway. It sounds like a win-win to me. References: 1. L. Nogueira, I. Ramirez-Sanchez, G. A. Perkins, A. Murphy, P.R. Taub, G. Ceballos, F.J. Villarreal, M.C. Hogan, M.H. Malek. (-)-Epicatechin enhances fatigue resistance and oxidative capacity in mouse muscle. The Journal of Physiology. 589.18. 2011 pp 4615-4631. 2. Gunnars, Kris. "7 Proven Benefits of Dark Chocolate." Authority Nutrition. 13 June 2013. Web. 11 June 2014. Knowledge = Power; Share the Power: -Train Smarter, Not Harder-  I would rather not admit how many times I have violated this principle but let's just say too many. I am at a crossroads again which inspired me to put pen to paper (or fingertips to keys) in hopes that someone can learn from my mistakes. For me, it all began a couple of weeks ago. Up until then I was in the best running condition at this time of year for the first time in a while. I had and still have high hopes for this season of racing but I've recently developed consistent lower shin pain seemingly out of nowhere. There have been no drastic changes in my training routines that would explain an injury such as this. It was also alarming to be fine one day and then experience consistent pain during the next run without an event to point to as the culprit. Now it should be noted the pain I was dealing with was not severe in any way but having a consistent sensation of pain and discomfort on every step was concerning. I have finally learned that it would be better to pay attention to my situation now instead of putting it off or ignoring it like I've done before. That's lesson #1 if you are keeping track: Take care of things early on instead of ignoring them or allowing things to fester and get worse. Having dealt with other injuries in the past I have also learned that continuing to run probably wasn't going to help the situation. Chances are it was only going to make things worse so as difficult as it was I decided to shut things down until I could resolve this particular issue. That's lesson #2: Sometimes you just need to stop as much as you don't want to. Even if there is a race or event coming up, it's better to give your body a chance to heal, recover and figure out the problem instead of just pushing through. I am not an elite athlete and I'm guessing anyone reading this isn't either so it is unlikely there is anything truly on the line that is worth risking further injury and delaying a return to your desired activity. As frustrating as it is, having the patience to take time off from running (even with a couple of events in the next month) and get to the root of the problem will pay dividends for the rest of my season and if all goes well, for the long term too. That's lesson #3: Be patient. Life is much better when you can live to fight another day rather than push through and be sidelined for much longer. Being "tough" and training harder ends up backfiring more often than not. Thank goodness I have the skills to figure things out and treat myself in most cases. Having finally learned these lessons the hard way, I should be able to solve my particular injury in the short term so that I am ready for the rest of the season. There is a time and place to train hard(er) and this is not that time. I am finally allowing my brain to help me train smarter which will help me get back on the trails and racing as soon as possible. So I encourage you to learn from my mistakes when training for whatever your endeavor may be. When healthy and especially when dealing with injury, take full advantage of those three pounds of tissue between your ears and train smarter, not harder. Knowledge = Power; Share the Power: After graduating from my physical therapy program I took it for granted that the general public truly knows what physical therapy is. I assumed (first mistake!) most people knew the basics since it is a common and relatively mainstream intervention for injuries...or so I thought. It also seems like most people have sought care from a physical therapist or know someone that has and yet there still seems to be a lot of misinformation out there. Now that I've worked with hundreds of clients and have been talking to many people within my community as I build my practice I have found that there is a huge spectrum of knowledge about what physical therapy is and who it can help as it relates to an outpatient style clinic. Here are some of my favorite thoughts I've heard over the past several years about physical therapy: You only work with people after they've had surgery. It's just a bunch of exercises. Chiropractors take care of the spine, you do everything else. You use cool gadgets like ultrasound and electrical stimulation. I thought physical therapy is hot/cold packs, massage and a couple of exercises. It's kind of like personal training, right? This is PT? This is a lot different than I expected! While there is some truth to a few of these statements, they are pretty amusing if you ask me because there is so much more to physical therapy than these ideas. I especially like the last one. The most common definition(s) you will see for physical therapists is something along the lines of someone who is licensed to evaluate, treat and/or prevent pain, disability, injury, movement dysfunction, disease and functional limitations using physical, mechanical or chemical means including but not limited to therapeutic exercises, mobilizations and/or manipulations, and modalities (cold/hot packs, ultrasound, electrical stimulation, etc.). The definition I prefer to use is physical therapists are neuromusculoskeletal experts (not to be mistaken with gurus), movement educators and performance enhancers (the legal kind). This means we are specialists in the human body, how it moves and how to address issues like pain, injury, strength deficits, dysfunction, disease progression and performance optimization among many others. No matter what exact definition you use for physical therapy they are very open ended which is great because it means we can work with virtually anyone. Through our training we have the knowledge to analyze and understand each component of the neuromusculoskeletal system including the brain, spinal cord, nerves, muscles, bones, joints, tendons, ligaments and connective tissues. More importantly, we understand how each of these components interacts with each other to influence and allow the human body to function. In order to address any and all of these components and their impact on the whole system, we have an extremely diverse skill set at our disposal. To begin with, we perform a thorough physical examination and assessment as it relates to a client's specific situation and complaints. We have a wide variety of tests and measures that reveal valuable information which is interpreted to develop a diagnosis, a treatment plan and a prognosis. As far as treatment is concerned there are several interventions we can choose from in our skill set. The specific mix of interventions will vary from clinician to clinician and from client to client depending on each individual case. They include: Education: This is quite possibly the most important part of treatment. First and foremost, it is our job to listen so that we know what to teach and explain. It is our job to teach anatomy and physiology, pain science, biomechanics, relaxation techniques...whatever is necessary to help our clients understand their bodies better. It is our job to dispel myths and fears so that the brain and body isn't in a constant state of stress and exacerbating any issues. It is our job to develop a plan and strategies for our clients so that they are able to help themselves and reach their goals. Manual Therapy: More often than not, physical therapists will be using their hands at some point. It is here that you will see many different philosophies and schools of thought. It is impossible to list all of the manual therapy variations but some of the general categories they would fall under are soft tissue mobilization like trigger point therapy, various styles of massage, active release technique and instrument assisted soft tissue mobilization to name a few, nerve mobilizations, joint mobilizations including chiropractic/thrust manipulations (depending on the state; legal in NY), stretching, and facilitation of movement to retrain motor control and movement quality. How each of these is performed and accomplished will differ from clinician to clinician. Exercise: This can be broken up into two subgroups even though they overlap quite a bit. The first being neuromuscular re-education which is a fancy way of saying movement retraining. Think balance, control, reaction and technique. Single leg balance is a perfect example of an exercise that would be considered neuromuscular re-education. The second group is therapeutic exercises and functional activities. Traditionally you can think of strength training, flexibility and range of motion exercises fitting into this category as well as activities of daily living like walking, stair climbing and carrying objects. You would obviously need good technique and control in order to accomplish these more traditional types of tasks. With any of these exercises, what sets physical therapy apart is they are prescribed and progressed very specifically to achieve certain goals that can be tested and measured. It is much different than a general fitness plan. Modalities: This is where the gadgets can be listed like electrical stimulation (my favorite), ultrasound and mechanical traction. It would also include things like heat and cold therapy. In many cases, these passive modalities are used for pain control which is very helpful and a good adjunct to treatment but they will rarely ever resolve the underlying issues. That is what the education, manual therapy and exercise is for. There are other times when modalities are used therapeutically like electrical stimulation to improve activation (and strength) of the quadriceps after knee surgery or cold therapy to reduce swelling and inflammation. Long story short, physical therapy is an extremely versatile and comprehensive solution to issues related to the neuromusculoskeletal system. You might even consider physical therapists to be jacks of all trades as we have a wide array of skills to choose from in order to help our clients reach their goals. So if you have neck or back pain, we can take care of you. If you just had surgery, come on in. If you feel like you have balance issues, we've got that covered. If you can't play your favorite sport, we would love to fix that. If you have pain/chronic pain and you can't figure out why, we'll figure out why. I could keep going. As you can see, physical therapy is an excellent first option if you have pain, suffered an injury, have functional limitations, etc. and you want to resolve these issues so that you can move better, feel better and live better. Knowledge = Power; Share the Power: This is a follow up to my previous post Patellofemoral Pain Syndrome: What Is It? For the purposes of keeping this discussion on the shorter side I am going to skip the smaller subgroup of people who fall into the category of actual structural factors like a shallow patellar groove or bony abnormalities and focus on the majority of people who have functional deficits that can change with treatment. In most cases, the knee joint itself is usually healthy and absent any major issues but is sensitive and irritated as a result of deficits elsewhere. Upon examination, these deficits most commonly show up in the hip and/or the ankle. There are occasions where the lumbopelvic complex can play a significant role as well but not as frequently. For these reasons alone it is highly recommended to consult with a physical therapist who will perform a thorough physical exam to decipher which factors are the probable culprits causing the patellofemoral pain. Going back to 1976, Nicholas et al shed some light on this issue and found that proximal thigh muscle weakness was strongly associated with a variety of lower extremity conditions, particularly with patellofemoral pain. (1) More recently, Peters and Tyson performed a systematic review of the literature addressing proximal (read: hip) interventions and their effectiveness in resolving patellofemoral pain. Based on their review, there is very good evidence suggesting that proximal exercises is an appropriate and effective treatment, especially early on. (2) If you are wondering why this is the case, think of the hip as the foundation of your leg. Weak foundations of any structure leads to all kinds of problems and the same can be said of the hip. By strengthening the muscles of the hip and thigh you provide a solid foundation for the joints below, particularly the knee, to function as they were designed to. Another way to say that is strong hip and thigh muscles are able to control the mechanics of the knee more appropriately which can eliminate whatever was irritating the patellofemoral joint. Another driving factor can be below the knee at the ankle joint. The foot can as well but that's another topic for another day. To illustrate my point I've attached a video courtesy of Chris Johnson: As you can see, mobility and range of motion issues at the ankle can have a dramatic effect on knee positioning and mechanics. Imagine if that is what your knee is doing every time you squat, negotiate stairs or get out of your car. My knee(s) (patellofemoral joint) would be pretty cranky too! Last time I checked, the knee is supposed to flex forward and back more than rotate in. It doesn't take a rocket scientist to realize that this situation would completely change the forces and stresses applied through the patellofemoral joint potentially resulting in knee pain. Since I did not work with this individual it is unclear whether the ankle range of motion limitation is due to a loss of joint mobility, calf tightness or both. Again, this is why it is highly recommended to consult with a physical therapist who can figure out the main factors. Either way, by addressing the ankle through mobilizations and/or flexibility work, there is a high probability of resolving issues further up the chain like patellofemoral pain. At this point you might be saying "well that's great information but what can I actually do about it, Greg?" The following is by no means an exhaustive program but a good starting point for patellofemoral pain: Hip (Proximal) Strength
Ankle Mobility There are many good techniques to improve ankle dorsiflexion but this is my go to for two reasons: 1) It works, and 2) You don't necessarily need the compression wrap for it to be effective. For some other ideas and if you have access to wraps or bands, Mike Reinold put together a bunch of them in his aptly titled article Ankle Mobility Exercises To Improve Dorsiflexion. Calf Flexibility Calf Stretch Steps and stairs make for great calf stretching. In either case, your forefoot is placed on the edge with a slight toe in of about 5 degrees. If your heel is touching the floor, keep your leg straight and lean forward until you feel a strong stretch. If you are using a stair, allow your heel to drop until the same strong stretch is felt. Hold for 60-90 seconds and repeat 3-5 times. If you've been experiencing anterior knee pain or have even been diagnosed with Patellofemoral Pain Syndrome, these exercises may provide with some relief but consider consulting with a physical therapist who can fine tune your treatment. References: 1. James A. Nicholas, M.D., Alan Marc Strizak, M.D., George Veras, M.B.A., M.P.A. A study of thigh muscle weakness in different pathological states of the lower extremity. American Journal of Sports Medicine. December 1976, vol. 4, no. 6, 241-248. 2. JS Peters, NL Tyson. Proximal exercises are effective in treating patellofemoral pain syndrome: a systematic review. International Journal of Sports Physical Therapy. 2013 Oct; 8(5): 689-700. Knowledge = Power; Share the Power: 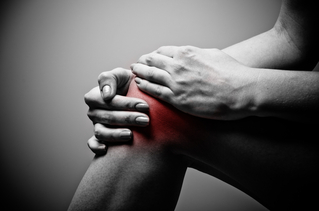 Recently, I've been asked a few times about Patellofemoral Pain Syndrome (PFPS) as well as a few clients walk into my office with complaints of knee pain so I thought I'd put together some information to try to clarify some of the issues related to this common ailment. A quick Google search of 'Patellofemoral Pain Syndrome' provides you with almost 350,000 results and after this post, you'll be able to add another one to that list. Try many of the other iterations like PFPS, patellofemoral pain, patellofemoral syndrome, runner's knee, chondromalacia patella, movie-goers knee, etc. and you'll come up with thousands more. So what does this all mean? Well it means there is a ton of information (and misinformation) about one of, if not, the most common knee injuries to plague athletes, weekend warriors, office workers, young, old...just about anyone. The first goal is to define what it is. The simple version is pain around and/or behind the kneecap (patella) as it articulates or touches the femur. That sounds pretty straightforward but it can present itself in a variety of ways which is why you will find so many definitions/results with a Google search and among healthcare practitioners. It is also part of the reason why it has been given the vague designation of a 'syndrome'. The truth of the matter is nobody knows exactly what causes it or what is happening at the patellofemoral joint when PFPS shows up to the party. All we know is that the end result is pain. Since there is no consensus on what is actually happening, that makes finding a solution more challenging than say a broken bone or muscle strain. Add other knee injuries that can be confused with PFPS like iliotibial band syndrome (ITBS, yet another syndrome and another post), patellar tendonitis and bursitis and one can see how a 'simple' definition can become a complicated issue to diagnose and resolve. Though quite varied from person to person, there are some hallmark symptoms, however, that can help narrow down the differential diagnosis. These commonly include, but are not limited to, pain with squatting, ascending/descending stairs, running and prolonged sitting. Sometimes joint effusion or swelling will be present but again, this is quite variable also. Granted, these are common complaints among other knee injuries as well so PFPS often becomes a diagnosis of exclusion due to signs, tests and subjective complaints that can help distinguish between issues like meniscus pathology, tendonitis, bursitis, ITBS, etc. Now this is where physical therapists make the 'big bucks' (I can dream, right?). It is nice to have someone walk into my office with cookie cutter complaints so that the solution is easy but honestly, that situation doesn't happen very often. Instead, I am able to use my training and knowledge in anatomy, kinesiology and biomechanics, muscle physiology, neuroscience and psychology to assess the incredibly dynamic system that is the human body and brain to formulate a conclusion as to why someone is experiencing pain, in this case patellofemoral pain. Through careful observation, specific tests and measures, and most importantly, listening to my clients, I can deduce the driving factors of someone's patellofemoral pain and customize a plan to resolve his/her pain and limitations. Quite often, there are multiple factors involved and it is my job to determine the best way to address them and sequence the plan to get my clients back to moving better, feeling better and living better. Stay tuned for my next post to learn about some of the ways patellofemoral pain syndrome can be resolved. Knowledge = Power; Share the Power:  Some of you may not be lucky enough to experience the invasion of the "polar vortex". I, for one, think this is what winter should be like and is reminiscent of winters past. You may think winter is too cold to begin with, let alone this particular winter, to get out there and log some miles on the roads and trails. I admit it's not for everyone but I find cold weather running rather invigorating. (I also despise treadmills so that limits my options anyway.) When you're talking about single digits, teens and into the 20's for air temperature, as it has been for my recent runs, speed work and interval training are not easy to do. Running faster especially if there is any kind of wind automatically makes it feel colder so it usually isn't the most enjoyable thing to begin with. Physiologically it is generally more difficult because your body uses more energy (read: oxygen) to maintain its core temperature and muscle efficiency decreases. (1) For most people this means more work for the same results in warmer temps. So what is a runner to do? Instead of hammering out intervals, winter can be a great time to focus on the fundamentals of your technique as it can have a dramatic effect on your performance. After that initial shock of the cold air, I like to start at the top and analyze all the way to the bottom: For me that means using my ears and listening to my cadence first. If you missed my post about the importance of your auditory organs as a runner you can read that here. Your cadence should sound relatively symmetrical regardless of foot strike preference. (That's another topic for the future.) How's your head position? Straight and stable? Good. What about your shoulders? Are they back and relaxed allowing you to maintain an upright posture and promote good lung function or are they tense and shrugged up to your ears? No bueno if it is the latter. How are your hands? Clenched like a death grip and creating tension throughout your whole upper body or gently flexed like you're holding an egg? What are your arms doing? Are your elbows comfortably bent? Is your arm swing compact and moving forward and back for the most part rather than side to side? Is one arm doing something the other arm isn't?? This is often a place where energy is wasted as the arms can do interesting things and take away your forward momentum. Onto the lower body. Are you getting hip drive with every step? Is one knee clipping your leg with each swing...maybe both? Are your feet clipping your legs...maybe one more than the other? Hint: this will waste energy and efficiency also. What's going on when your foot hits the ground? Does it feel like (sound like) you're landing relatively symmetrical each step? Are you transitioning all the way through the big toe so that you have maximal forward propulsion every step? Do you find you push off more to the inside of your foot? This is another example where energy can be lost and decrease performance. There you have it...a quick checklist of things to dial in on as you rack up your mileage so that you come out of winter as an efficient runner ready to dominate your goals and races. This is by no means an exhaustive list as each component could be broken down further if need be and usually requires another pair of eyes for observation and analysis. In most cases everything will probably check out and you can be on your merry way to enjoying some cold weather runs. If something is off or you're dealing with a nagging injury that won't go away no matter what you do, consider consulting with a physical therapist knowledgeable in running injury and performance. Happy running, embrace the polar vortex and see you out on the trails! References: 1. Nimmo, M. Exercise in the cold. Journal of Sports Sciences. 2004 Oct; 22(10) pp:898-916. "Variety's the very spice of life." - Poet, William Cowper Recently, I saw a picture of my friend's dog, Sammy, in a ridiculous position (one of many at this point) and my first reaction was to laugh as usual and shake my head. I'm pretty sure we've all seen something like this at one time or another. Immediately my next reaction was "How is that comfortable?" As you can see above, most of the time he is lounging on big fluffy pillows but it still looks like an awkward position. But then it got me thinking, maybe it isn't so awkward after all. Maybe this kind of variety is a good thing to do. Clearly it doesn't seem to faze him as he's good to go after he gets up and stretches it out a little bit just like every other dog you've ever seen. Maybe we can learn something here. Granted, humans are not dogs and dogs are not humans (even though we treat them like that sometimes). However, we are made of the same stuff like bone, muscle, nerves, ligaments, etc. so maybe it isn't such a bad comparison in this instance. How many times are you told some position or posture is bad for you? Doctors, physical therapists, chiropractors, yogis, the internet are constantly telling you what you should and shouldn't do. There are obviously some basic guidelines that are worth practicing but they may not have to be so strict. I will be the first to say that I am guilty of saying something similar to my clients over the years but more recently I've added a caveat and I think Sammy does a great job of illustrating my caveat. It goes something like this: "Just don't do it 100% of the time." None of Sammy's positions are the same so he is most definitely not doing the same thing 100% of the time. In general, consistency, repetition and overuse are what tend to get people in trouble more than a specific position or posture itself. They end up sitting the same, standing the same, laying on the same side to watch television often for prolonged periods of time. As you can see above, Sammy doesn't subscribe to doing the same thing over and over again. He's living the dream of variety in his life (at least in sleeping positions). Maybe all of these different positions stimulate his nervous system (his brain) and the tissues of his body since nothing is ever the same. Maybe it is important to take advantage of the full range of motion of each joint at some point during the day. Maybe it is important to stretch muscles in a variety of positions throughout the day. The living body, dog or human, is extremely adaptable and can handle all kinds of positions and postures. Think break dancers and Cirque du Soleil performers. They can do all types of "crazy" and "awkward" things with their bodies and they make it out alive just fine. Just don't do the same thing 100% of the time. Chances are your body welcomes the change and variety and will be better in the long run. So don't beat yourself up if you find yourself in a "bad" position on a super soft sofa that was really comfortable. Don't beat yourself up if you find yourself slouching as I just was until writing this sentence. Just don't do it 100% of the time and you will be ok. When you do catch yourself doing something all of the time, take some advice from Sammy: Change things up and add some variety to your life...or napping position at the very least. Your body will thank you for it. Remember, variety's the very spice of life (in more ways than one).
 If you are local to the New Paltz area or even if you are visiting family and friends, chances are pretty good you've heard of a little event called the New Paltz Turkey Trot at this point. It has grown immensely over the years and is much more than just a 5k race/walk. It has become a great tradition every Thanksgiving for friends and family to get together for a fun community event before diving into all the deliciousness that follows the rest of the day. Chances are you'll probably run into a friend or two you haven't seen in a while as well. It is also an important fundraiser for Family of New Paltz which provides invaluable services for those in need. This year's Trot is shaping up to be a chilly one with some wind to go along with it but don't let that scare you away! Whether it is your first Turkey Trot, first 5k ever or you can't remember how many 5k's you've done, it is a fantastic event and a flat, easy course. So come join the fun, support a great organization that is so important to the community, and burn some calories before digging into your feast! Registration is still open on Wednesday at the Jewish Community Center from noon-6pm or the morning before the race at Water Street Market. Race is set to go off at 9am. For all information and details about the Trot, you can head over to their website: www.newpaltzturkeytrot.com/index.html See you race day! What do you listen to when you run? Are you singing along to your favorite '80s mix, rocking out to Metallica's greatest hits or catching up on your favorite podcast? All of these actually sound like pretty good options but do you ever take your earbuds out and just listen to yourself run? There are a variety of ways to analyze running performance but using your auditory organs isn't commonly on that list. And unlike some of the others like video analysis or a biomechanics evaluation, you can perform an auditory analysis on your own and on any surface inside or out. Sound is a powerful tool and is something I use often with my clients and certainly for myself when I am running.
For the purposes of this discussion, the assumption is that there are no significant asymmetries (structural or functional) or previous injury, prosthesis or orthosis that prevents symmetry of the body in stance or with movement. The first, and probably easiest thing, you can key in on is the sound of your cadence. You should sound like a metronome when your feet hit the ground. There should be equal time (or silence) between each foot strike as well as equal time (or sound) when each foot is in contact with the ground. The latter can be a little more difficult to discern because the transition over the foot is generally quite quick. If there is a difference between foot strikes, then that may suggest possible issues like inefficiencies in your running mechanics or imbalances in higher joints which could lead to nagging injuries or limit your mileage or pace. Without overhauling your technique see if you are able to tweak your cadence first so that it is more even the next time you run. Assuming that your cadence is symmetrical, the next sound(s) to listen to may be a little more challenging: how your feet actually strike the ground. Are you a heavy hitter with a solid impact each time or are you light like a gazelle? Is one foot heavy and the other light? Depending on how light or heavy you land (and also which source you read), you are landing with 1.5 to 3 times your body weight on a flat surface. That is a lot of energy and it has to go somewhere. The Earth is certainly not going to budge which means all of that energy is translated into your body. If you land on the heavy side, injuries could pop up generally more structural in nature like stress syndromes and stress fractures. If you land exceptionally light or soft, this could actually mean that you're absorbing so much energy that you lose some efficiency in your technique and soft tissue injuries like tendonitis is more likely to show up. For instance you may bounce up and down more with each step rather than using that energy to move forward. There's a delicate balance between landing too hard or too light and listening to your foot strike can help you find that sweet spot. If you're lucky, you've got it already. Another sound to listen for is the foot slap. For those unfamiliar it almost sounds like two impacts when you land: first with the heel followed quickly by a loud "slap" by the forefoot. This is not to be confused with regular heel striking with a smooth transition versus other styles of landing. (That is a completely different discussion which will be covered in future posts.) This pattern generally describes someone who is over striding. When the foot and leg are too far out in front of your body and center of mass, it is difficult to transition smoothly and it is a less stable position which results in the distinct foot slap sound. The "easy" fix for this is to shorten your stride which may feel a bit awkward at first but long term will feel more smooth and comfortable when you run. Lastly, breathing. This encompasses all runners regardless of your cadence or foot strike patterns. Without getting into any specific technique (there are several out there but this is also a different discussion for another day), the one thing that they all have in common is rhythm. Make sure your breathing is consistent and has a rhythm to it so that you are constantly getting the oxygen you need to perform. Should there be any noticeable differences that persist and you are unable to correct them yourself or you develop pain, consider consulting with a physical therapist knowledgeable in running injury and performance to review your technique and history. See you out on the trails! If you found this to be helpful, please share! |
Dr. Greg Cecere
Your personal physical therapist, movement educator and knowledge dispenser. Newsletter Sign Up
Enter your name and email to get Momentum PT's Movement Manual delivered straight to your inbox! It's your free monthly newsletter and guide to moving better, feeling better and living better! Archives
April 2017
Categories
All
Disclaimer:
The contents of this blog is meant for educational purposes only. Momentum Physical Therapy of New Paltz and Dr. Greg Cecere are not responsible for any harm or injury that may occur due to any information on this blog as it is by no means a substitute for a thorough evaluation by a medical professional. |
|
Momentum Physical Therapy of New Paltz, PLLC. Copyright © 2013-2023. All Rights Reserved.
Disclaimer: The contents of this site is meant for educational purposes only and utilization of any of the material is a personal choice. Momentum Physical Therapy of New Paltz and Dr. Greg Cecere are not responsible for any harm or injury that may occur due to those choices. This site is by no means a substitute for a thorough evaluation and guidance by a licensed medical professional.
|








 RSS Feed
RSS Feed
